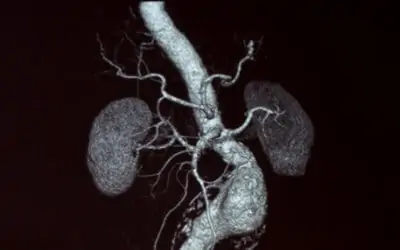
The aorta is the main blood vessel which brings blood from your heart to the rest of your body. As the aorta passes through the abdomen, it gives off branches to all of the internal organs. Just below the level where the arteries to kidneys come off is a special segment of aorta which can expand as we grow older to form an aneurysm or dilatation of the main vessel. The incidence of aortic aneurysm disease here in the Southeast appears to be one of the highest in the nation. Therefore a review of the pathophysiology or causes of this problem and the surgical treatment options seems to be timely.
The etiologies of aortic aneurysms have long been thought to be that of degeneration of the aortic wall, infection, dissection, smoking or splitting of the vessel wall due to high blood pressure. Although all of these causes most probably play a role, new research seems to shed light on the underlying cause. This is important news for patients with aneurysms because the clinical manifestations and natural progression of aneurysms make them serious problems that can lead to disability or death in many patients.
Beginning in 1990, scientific attention began to focus on a specific mutation of a gene that encodes for type III Procollagen. This gene exerts control over the production of collagen and elastin in the blood vessel wall. Both collagen and elastin have, as their main function, the strength of the vessel wall. Therefore, if you are born with this specific gene mutation, the aortic wall may be weak and an aneurysm may begin to grow silently as you get older. Many of the known risk factors for aortic aneurysms (such as smoking, hardening of the arteries and high blood pressure) act in non specific ways. This may be the first evidence that susceptibility to aortic aneurysms may arise from a single recessive gene and most importantly, this same gene can be transmitted by you to your offspring and successive generations.
An aneurysm is a localized irreversible dilatation of the artery. The normal size of the aorta is 2.5 cm. A 50% increase in the size of the vessel is the usual threshold for naming the aorta as having an aneurysm. The risk of rupture and death as the aneurysm enlarges can be accounted for by two factors: (1) the larger the aneurysm, the greater the loss of strength of the aortic wall. In scientific terms, the Law of LaPlace says that tension equals pressure x radius. So as the aneurysm gets bigger or the radius increases, the tension of the wall increases until the aorta ruptures. A recent study of the risk of rupture in aortic aneurysms revealed an 8% risk of rupture in aneurysms less than 4 cm. Remember, the normal size is 2.5 cm. In aneurysms between 4.1 cm and 7 cm, the risk increases to 25%. From 7.1 cm to 10 cm, it increases yet again to 45%. A new study on families of aneurysm patients has shown that first degree relatives of patients with aneurysms have a 19.2% chance of having an aneurysm vs. 2.4% chance in non aneurysm bearing families.
The presenting symptoms of an aneurysm which is about to rupture man vary. Most patients however, experience a severe abdominal pain just below the breast bone which radiates into the back. Many patients describe this pain as the sensation of being shot in the abdomen by an arrow. Abdominal aneurysms are diagnosed 70% of the time by palpation by the family doctor as part of a physical exam. Abdominal ultrasounds and CAT scans are then used to confirm the location and the size of the aneurysm. Coexisting disease is very common and must be addressed. Coronary artery disease, high blood pressure and lung disease exist in a least 50% of patients with aneurysms. Dye tests such as aortography may also be used to locate the renal artery branches and other vascular anomalies.
Recommendations:
1) If I am found to have an abdominal aneurysm I will need an ultrasound or CAT scan or both to determine its size and location.
2) If the aneurysm is 5 cm or larger and I am otherwise healthy and a candidate for surgery as determined by my cardiologist or internist, then I should get a stress echocardiogram to assess my heart function.
3) If the aneurysm is less than 5 cm and I am not symptomatic, then screening ultrasounds every 3 to 6 months should be done. Most commonly, aneurysms expand about 0.4 cm per year.
4) Finally, if surgery is recommended, the surgeon will replace the segment of aneurysm with a dacron graft and I should be back to work in about a month. Newer techniques of endovascular repair are available for selected patients and this can be determined by my surgeon.
