SUMMARY: Decubiti, or pressure sores, occur in individuals who have restricted mobility and intrinsic susceptibility to tissue damage from malnutrition, disease states, and other risk factors. If they are not prophylacti-cally managed by their care givers, by relief from pressure, friction and shear stress, skin and subcutaneous tissue damage eventuate and pressure ulcers develop. These ulcers are divided into 4 stages, depending on their depth and the tissues involved, I.e., skin, subcu tissue, muscle, bone, tendon or joint capsule and the association of tissue destruction and necrosis. The best treatment is prevention. Failing this, the ulcers are treated with cleansing solutions as well as debridement with enzymatic gels, pressure irrigation, sharp surgical dissection and grafting, as well as various adjunctive therapy. The ulcer tissue, once healed is never the same as before and is inherently weaker and susceptible to future breakdown. Complications from loss of limb to loss of life may occur.
TEXT: Decubiti consist of the breakdown of skin and underlying soft tissue at areas of sustained pressure, usually over bony prominences, especially in people, who are elderly or are immobile, from such things as paralysis, coma, sedation etc. That’s why Decubiti are often referred to as Pressure Ulcers or Bedsores.
Decubiti are divided into 4 Stages: (NPUAP and AHCPR criteria)
1.) Stage 1- Nonblanchable erythematic of intact skin
2.) Stage 2- Superficial or partial thickness skin loss
3.) Stage 3- Full thickness skin loss with Subcutaneous damage. The ulcer extends down to the underlying fascia.
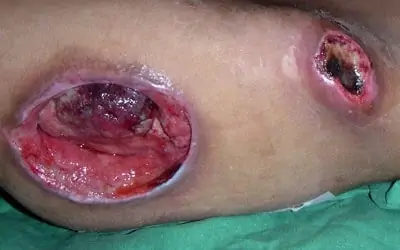
4.) Stage 4- Full thickness skin loss with extensive destruction accompanied by tissue necrosis with damage to muscle, bone, tendon or joint capsule.
These stages do not necessarily worsen or improve, when treated, through one stage to the next, but can leap from one stage to another. And an ulcer cannot be accurately staged until it’s Escher (scab) is removed.
Pressure ulcers are prone to occur in the lower body, particularly the bony prominences and weight bearing surfaces of immobile persons, especially over the Sacrum, Hips, and Heels.
Pathophysiology
Whenever pressure interrupts the blood flow to the skin and subcutaneous tissues, ischemia develops. After a minute or so, changes develop in these tissue. The skin may become red and blanchable. Before long, the blanching no longer is elicited and the damage becomes irreversible, supposedly, from capillary extravasation of plasma and red cells. The subcutaneous tissue is even more sensitive to ischemia. Therefore when the skin is red (hyperemic) and nonblanchable, the underlying subcutaneous tissue is probably even more damaged, such that, pressure ulcers are often more extensive than they appear superficially.
Risk Factors
Both intrinsic (patient factors), and extrinsic factors are implicated in the development of Pressure Ulcers. The intrinsic factors include immobility, impaired cognitive ability, limited functional ability, fecal incontinence, impaired sensation, and diminished level of consciousness. Laboratory abnormalities, such as hypoalbuminemia, a decreased lymphocyte count, decreased body weight, and inadequate dietary intake (all indications of malnutrition) are risks. Age greater than 75 y/o do to changes in skin and subcutaneous integrity and circulation, appears to increase risk. Stroke, Parkinson’s disease, fractures, diabetes, sepsis, and prior ulcers also increase the risk. Fecal and, in some cases, urinary incontinence may contribute. Any condition that increases the metabolic rate, such as hyperthyroidism, takes nutrition away from the skin and subcutaneous tissue and increases the risk.
The extrinsic factors are largely self evident, being do to pressure, friction, shearing and moisture. The pressure from prolonged sitting or lying will rise above the normal capillary filling pressures and the circulation will be obliterated. Ultimately cellular death will occur and an ulcer will eventuate. When an individual is pulled across a support surface, friction will occur and skin tears, abrasions, superficial erosions and blisters may occur, break down, and develop into ulcers. Sliding causes angulation of perforating arterioles, which may compromise circulation. Moisture softens the stratum corneum and increases the risk of injury from friction, secondary to maceration. The presence of bacteria associated with unclean and acidic conditions from stool or urine can aggravate denuded skin areas.
Complications
Pain, secondary infection, systemic infection, loss of limb, osteomyelitis, and death are all possibilities when pressure ulcers are overlooked and not treated aggressively and appropriately. When ulcers do occur, the proper selection of therapies from among those many available, can help prevent these potentially devastating complications.
Treatment
Prevention is the most important part of decubitus care. Daily examination of the skin to note any breakdowns; turning the patient from side to side every 2 hours, day and night; encouraging ambulation, if possible; avoiding sitting for long hours; monitoring appetite, caloric intake, weight loss, ideal body weight, and serum protein and serum albumin (a weight loss of 8 lbs/quarter or > 10% of body weight within 6 mos. is critical to suggest malnutrition); monitoring incontinence of urine or stool, timely treatment of infections all are important and necessary to prevent pressure sores in this group of patients. The timely institution of prophylactic and corrective measures can help prevent or slow the progression of pressure ulcers.
Unfortunately, once the skin starts to break down, it’s doubly tough to turn back the clock. Even when the decubitus ulcer is healed, the character of the subcutaneous tissue and the skin are not back to normal, and have an enhanced tendency to break down again with less provocation. Treating the associated pain, covering the wound, and diminishing the tissue load are good initial approaches to the decubitus problem. The underlying goal is to preserve intact skin and to prevent deep tissue damage. Often, once the decubitus is detected, there is more damage underneath the skin than is suggested by the skin’s appearance. Some authorities preach that Decubitus Ulcers start deep and extend upward in a pyramid fashion.
Once the pressure ulcer has reached Stage II, cleansing with isotonic sodium chloride solution followed by use of hydrocolloid wafers, semi permeable foam dressing, or a polyurethane film (which is changed every 3 to 7 days). When a Stage III or IV is encountered, the Debridement of the dead and eschar tissue is mandatory, as this tissue will encourage secondary infection and impede healing. This debridement may be implemented, if minimal necrotic tissue is present, with autolytic, mechanical (wet-to-dry dressing), enzymatic, or, by surgical methods. Cleansing with isotonic sodium chloride solution using high-pressure may be helpful. The wound is then dressed with hydrocolloid wafers and semi permeable foam dressing if shallow and wet gauze to fill the depression if the wound is deep and clean. Necrotic debris or devitalized tissue must be removed, either by wet-to-dry dressing or surgically. An absorptive dressing is useful if there is excessive exudates present.
Debridement is devided into autolytic, mechanical, enzymatic and sharp (surgical ) types. In the Autolytic variety, the ulcer covering allows the accumulation of tissue fluids that contain macrophages, neutrophils, and enzymes, with selectively remove bacteria and devitalized tissue. The Mechanical Debridement is implemented by a moist dressing which is allowed to dry and adhere to tissue at the wound base. Topical enzymes are available to remove devitalized tissue and high pressure irrigation helps dislodge debris. Sharp Debridement is done with surgical instruments to remove any nonviable tissue, necrotic tissue or Eschar.
Since bacteria always colonize Stage II, III, and IV ulcers, removal of necrotic and devitalized tissue is paramount in the healing process. Topical antibiotics may then be helpful. IV antibiotics are needed if advanced cellulites, bacteremia, sepsis or osteomyelitis is suspected.
Surgical Repair
If the Stage III or IV ulcers fail to granulate in and heal, surgical repair may be necessary. Direct closure may be a possibility, although the lesions are generally too large for same. In that case, skin grafts, skin flaps, musculocutaneous flaps, and free flaps have been successful.
Adjunctive therapy
Hyperbaric oxygen, electrical stimulation, infrared or ultraviolet light, low energy laser irradiation, ultrasound therapy, and application of growth factor topical agents have proved of some value in the hands of some practitioners. Even Maggots have proved useful in debridement. At present, only electrical stimulation has been recommended by the AHCPR as an adjunct to the conventional treatment of decubitus ulcers.
Re: Post Grad Med; 2003, May;113(5):77-8,81-4,88-90
Todays OR Nurse. 1994 Nov-Dec; 16(6):33-40
J Fam Pract. 1997 Apr; 44(4):361-8
Agency for Health Care Policy
National Pressure Ulcer Advisory Panel
